In this article, we explore the incidence of cancer in pregnancy, common barriers, and tips for primary care clinicians to help birthing people diagnosed with cancer, and their families.
Incidence
Cancer during pregnancy is rare. Estimates vary, but research by the National Cancer Registration and Analysis Service (2018) estimates that approximately 1 in every 1000 pregnancies are affected. When this statistic is measured against the UK birth rates over the past 4 – 5 years, this equates to two women per day receiving a diagnosis of cancer during or within 12 months of pregnancy (Wallroth, 2019).
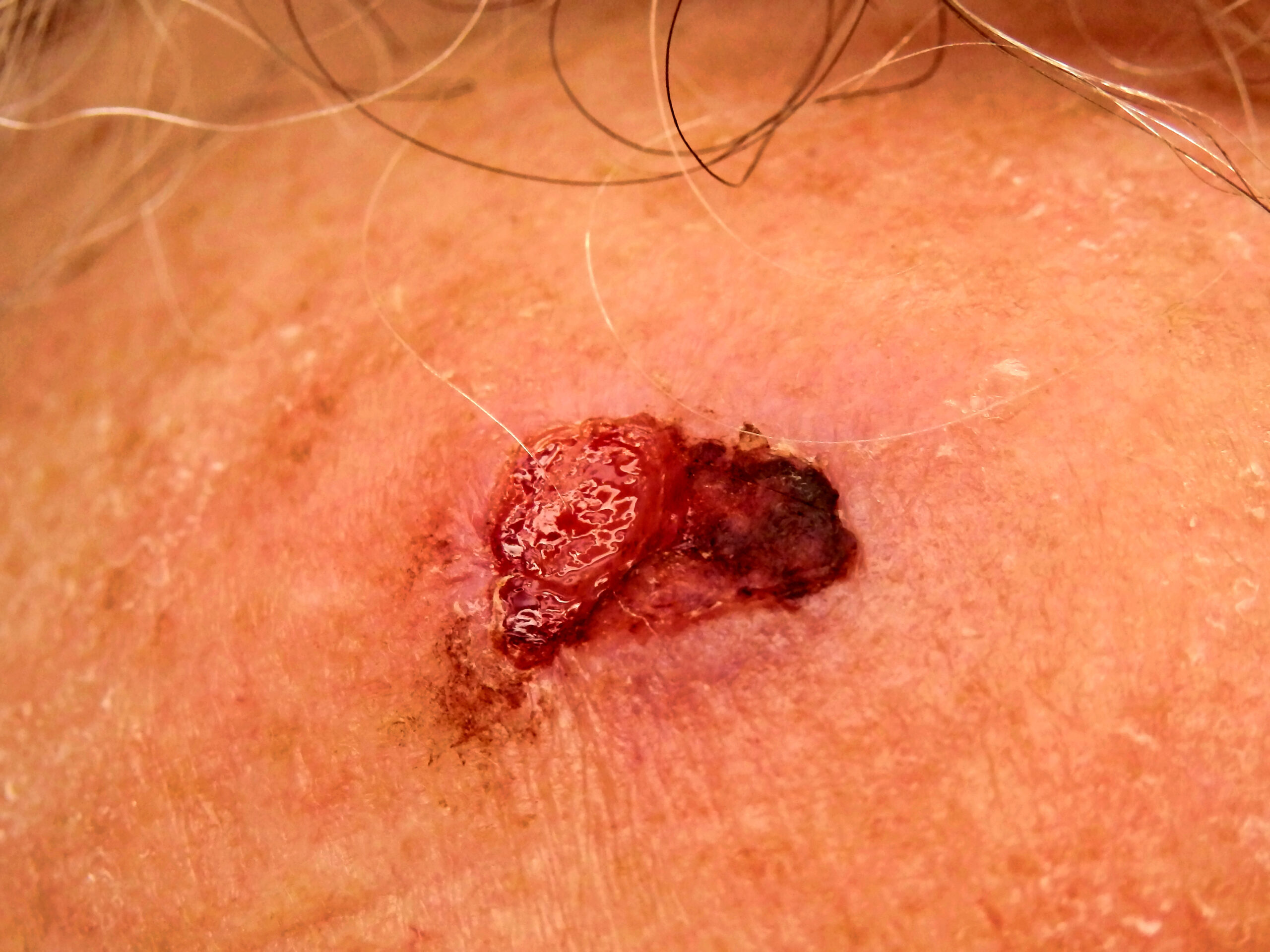
Often, the more common cancers that occur during pregnancy are the cancers that we see affecting women of child-bearing age and the two events coincide. Common cancers can include thyroid, lymphoma, leukaemia, breast, cervical and melanoma. There is also a specialist and separate form of cancers named Gestational Trophoblastic Tumours (GTT) which are a rare group of diseases in which the tissues formed in the uterus following conception grow abnormally to form a tumour.
How can we help?
So, as primary care clinicians what can we do to support women and their families overcome the obstacles to a cancer diagnosis? In our latest Cancer Conversation, we spoke to clinicians and Mummy’s Star, a charity dedicated to women and birthing people diagnosed with cancer during pregnancy or within 12 months of giving birth, and their families, to find out more.
See the symptom, not the pregnancy
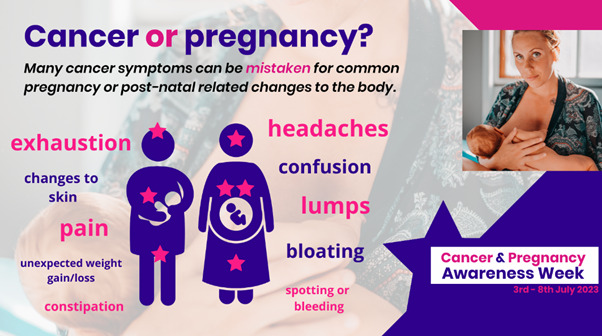
Diagnosis in pregnant women can be delayed as many cancer symptoms can be mistaken for the normal physiological pregnancy or post-natal related changes to the body. This is often referred to as symptom shielding, with common symptoms including exhaustion, changes to the skin, lumps, bloating, and more. Promoting the patient’s body awareness and confidence to voice a concern is often essential for an early diagnosis.
Robust safety netting
It is important that GPs discuss a robust safety netting pathway when women present with new symptoms in pregnancy and have a clear plan of when to review or refer the patient if symptoms don’t resolve. It is also important to remember, that if a woman is in her second or subsequent pregnancy and is presenting with symptoms that feel abnormal for her, that this is taken seriously and that the GP has a lower threshold to instigate a referral.
Investigating
A sensible piece of advice is to consider the symptoms in isolation from the pregnancy and investigate patients in the same way as other patients presenting with suspected cancer symptoms. Remember as women become pregnant later in life the risk of cancer rises.
Treatment reassurance
In GatewayC’s recent Cancer Conversation centred on cancer and pregnancy, we spoke to Dr Richard Simcock, Consultant Clinical Oncologist, who shared:
“Often, one of the challenges is reassuring patients, sometimes patients that are disbelieving, that we can safely treat their cancer during pregnancy”.
In many cases, cancer treatment can be delivered without risk to the baby. More women are receiving cancer treatment during pregnancy, as fetal, neonatal, and short-term paediatric outcomes after cancer treatment are reassuring (Wolters et al, 2021). Chemotherapy, radiotherapy, and surgery are all treatment options that may be considered by the multidisciplinary team, during pregnancy. Treatment options, risk and impacting factors are also discussed with the patient and their families by the team.
However, it is important to note that some cancer treatments may harm the baby, especially during the first trimester, meaning treatment may be delayed until the second or third trimesters. To learn more, watch our Cancer Conversation.
Other tips
Each year Mummy’s Star runs Cancer and Pregnancy Awareness Week. This year, the charity promoted the ways that primary care clinicians can support patients to overcome the obstacles to diagnosis. Their tips are shared below.